Improved image quality and unified SUV results
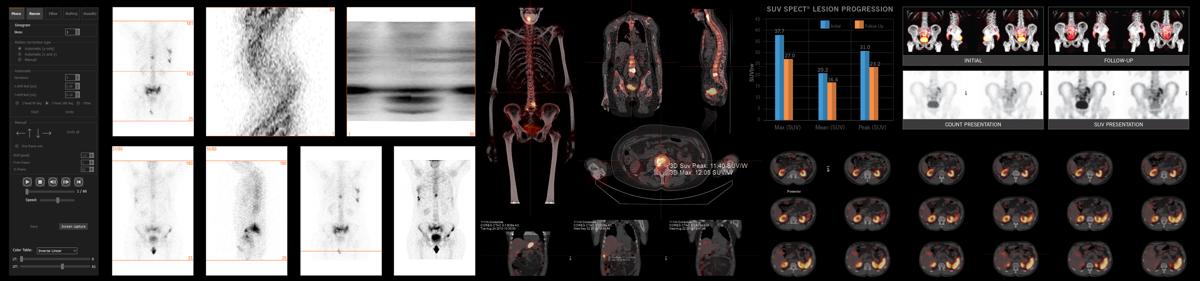
Leveraging the full potential of SPECT
Using software and hardware techniques, Hermia's SPECT reconstruction is optimized for speed and a wide range of procedures, radio-pharmaceuticals and collimators, making it possible to improve image quality while reducing dose and acquisition time for virtually any camera manufacturer.
See our white paper on Advanced Bone SPECT Reconstruction in Hermia
-
SUV for all radionuclides and all SPECT cameras
Ga-68; Ho-166; l-123; l-131; ln-111; Kr-81m; Lu-177; Tc-99m; TI-201; Y-90
-
Fastest reconstruction on the market
Thanks to the GPU computing capabilties, Hermia is able to reconstruct SPECT up to 24 times faster than multi-threaded CPU implementation (5)
-
Full collimator modelling
Advanced resolution recovery achieves excellent image quality for the most difficult radionuclides like l-131; l-123; Y-90; Ho-166 (6)
-
Accurate planar reprojection
Generate accurate planar images from the reconstructed SPECT
Hermia SPECT Reconstruction
”We have leveraged this technology to reduce our injected activities while maintaining diagnostic image quality - even with older imaging equipment.”
- Ran Klein, PhD, The Ottawa Hospital
Hermia SUV SPECT®
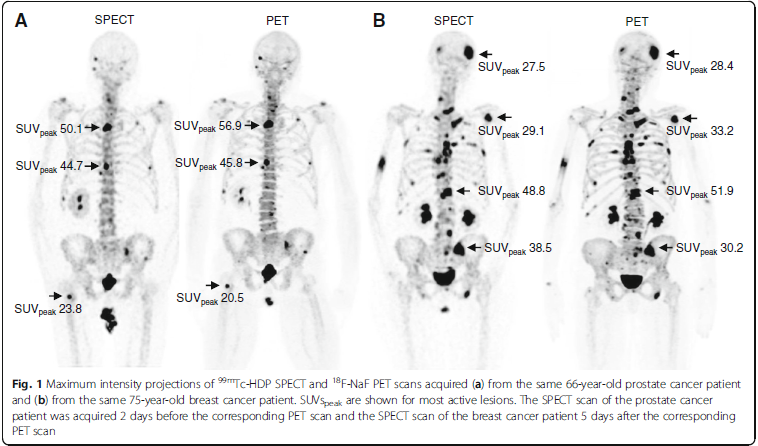
The advanced reconstruction algorithms from Hermia SUV SPECT® enable conversion of the recorded counts per voxel into activity per unit volume with SUV calculations, providing essential and accurate quantitative results. Numerous clinical and technical validation publications support the accuracy and reliability of the software (1-4).
Hermia's complete reconstruction package include tools for quality control, motion correction, collimator response, attenuation and scatter correction, attenuation map registration, and post-filtering. Ready for SPECT-MR, SPECT-CT, SPECT Reconstruction and SPECT Quantification.
References
- Arvola S, Jambor I, Kuisma A, Kemppainen J, Kajander S, Seppanen M, Noponen T. Comparison of standardized uptake values between 99mTc-HDP SPECT/CT and 18F-NaF PET/CT in bone metastases of breast and prostate cancer. EJNMMI Res. 2019 Jan 24; 9(1): 6
- Kangasmaa TS, Constable C, Hippelainen E, Sahlberg AO. Multicenter evaluation of single-photon emission computed tomography quantification with third-party reconstruction software. Nucl Med Commun. 2016 Sep; 37(9): 983-7
- Hippelainen E, Tenhunen M, Maenpaa H, Sahlberg A. Quantitative accuracy of 177Lu SPECT reconstruction using different compensation methods: phantom and patient studies. EJNMMI Research (2016) 6:16
- Kangasmaa TS, Constable C, Sahlberg AO. Evaluation of quantitative 1231 and 1311 SPECT with Monte Carlo-based down-scatter compensation. Nucl Med Commun. 2018 Dec; 39(12): 1097-1102
- Bexellius, Sahlberg A. Implementation of GPU accelerated SPECT reconstruction with Monte Carlo-based scatter correction. Ann Nuc Med, 32(5): 337-347, 2018
- Porter C, Bradley K, Hippelainen E, Walker M, McGowan D. Phantom and clinical evaluation of the effect of full Monte Carlo collimator modelling in post-SIRT yttrium-90 Bremsstrahlung SPECT imaging. EJNMMI Research (2018) 8:7

Request more info or a demonstration
We would be happy to show you the many possibilities offered by HERMIA through a demonstration or to answer any questions you might have.
To support all your clinical workflows
Browse to read more about all the many possibilities offered by Hermia– our ALL-IN-ONE state-of-the-art software suite. You can pick and choose the specialities and tools adapted to your current clinical needs and scale up whenever new possibilities arise.
-
Read more
PET/SPECT/CT/MR Reviewing
Hermia offers a high-performance and highly intuitive software for the display and analysis of PET/CT, SPECT/CT and PET/MR.
-
Read more
Oncology
Handle all your oncology work from diagnostic imaging, reporting to therapy for all modalities and scanners.
-
Read more
Theranostics
Theranostics is a very promising personalized approach to treating cancer, using diagnostic imaging to identify if target receptors are present on cancer cells, followed by precision internal radiation treatment that targets these receptors.
-
Read more
Dosimetry
Dosimetry is becoming more important as nuclear medicine is moving towards therapy. Regardless of where your practice is at, we have got you covered with the tools you need to easily plan personalized radionuclide treatment for your patients.
-
Read more
Neurology
Hermia Neurology has a fully automated 'single click' workflow. Data is processed, quantified and displayed within seconds with minimal user intervention.
-
Read more
Pneumology
Anatomically accurate lung function and volumes with Lung Lobe Quantification and fast and easy Lung SPECT VQ image display and analysis
-
Read more
Cardiology
State-of-the-art product line for cardiology, including third-party software with Invia Corridor4DM and Cedars-Sinai Cardiac Suite.
-
Read more
IT Solutions
Our Software and Hardware solutions have been designed to integrate seamlessly to your current workflow and systems and to offer the possibility to grow with your organization. The result is an improved user experience where the systems work for the user and not the other way around.